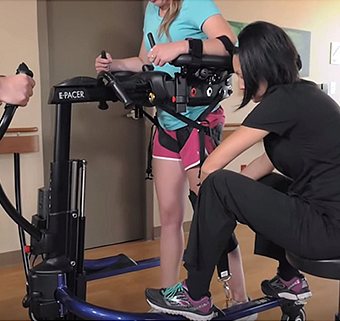Three Safe Patient Handling and Mobility (SPHM) Myths Debunked
| October 2025 Patient transfers are a routine part of all therapy interventions. These might involve assisting someone from a wheelchair to a mat table or parallel bars or helping a child into a gait trainer. However, these transfers put therapists and caregivers at high risk for work-related injuries, particularly lower back pain.1 Statistics show that injury rates significantly increase for caregivers who engage in manual patient lifting, transferring, and repositioning activities beyond the 35-lb patient lifting maximum recommended by the National Institute of Occupational Safety and Health (NIOSH).2,3 The consequences extend beyond pain and disability. Injured therapists may miss work, struggle to provide adequate patient care, and sometimes leave the profession entirely.3,4
Patient transfers are a routine part of all therapy interventions. These might involve assisting someone from a wheelchair to a mat table or parallel bars or helping a child into a gait trainer. However, these transfers put therapists and caregivers at high risk for work-related injuries, particularly lower back pain.1 Statistics show that injury rates significantly increase for caregivers who engage in manual patient lifting, transferring, and repositioning activities beyond the 35-lb patient lifting maximum recommended by the National Institute of Occupational Safety and Health (NIOSH).2,3 The consequences extend beyond pain and disability. Injured therapists may miss work, struggle to provide adequate patient care, and sometimes leave the profession entirely.3,4
Strong research linking manual patient lifting to injury risk gave rise to the Safe Patient Handling and Mobility (SPHM) movement. SPHM advocates the use of powered lifts, mechanical aids, and transfer devices to replace all unnecessary and hazardous manual approaches in patient care and rehabilitation. Major healthcare organizations have adopted SPHM principles – including the Veterans’ Administration, the Association of Rehabilitation Nurses, the American Physical Therapy Association, and the American Occupational Therapy Association. These organizations recognize that safe patient lifting equipment effectively reduces on-the-job injuries.5 Despite this support from major organizations, safe patient handling has seen slow adoption.6 This likely stems from three common misconceptions.
Three Safe Patient Handling Myths
1. Body Mechanics Will Protect You
In the past, physical therapy, occupational therapy, and nursing schools focused on teaching manual lifting techniques. Educators believed that proper body mechanics could prevent injury during transfers, regardless of the patient’s or caregiver’s size or strength. This approach is fundamentally flawed. Current biomechanical research shows that good body mechanics alone cannot prevent work-related musculoskeletal disorders.
Landmark research by Marras and colleagues measured the forces acting on caregivers’ spines during patient transfers. Even experienced caregivers using standard techniques, such as a two-person transfer with a gait belt or a one-person “hug” transfer, regularly exceeded safe spinal force limits.7 Therapists face even greater risks during therapeutic activities like prolonged gait training sessions, as they expose their spinal tissues to high mechanical loads for extended periods.1,5,8,9
 Additional research by Daynard confirmed these findings and showed that safe patient handling devices significantly reduced peak spinal compression values during the transfers.10 Further studies reinforced that SPHM equipment prevents far more injuries than manual lifting techniques.5,11,12
Additional research by Daynard confirmed these findings and showed that safe patient handling devices significantly reduced peak spinal compression values during the transfers.10 Further studies reinforced that SPHM equipment prevents far more injuries than manual lifting techniques.5,11,12
Body mechanics still matter. Maintaining proper posture is a good habit and supports safe patient care – especially when positioning and assisting patients into and out of lifting devices. However, believing proper body mechanics alone can prevent injuries is a dangerous myth that puts caregivers at unnecessary risk.
2. Professional Awareness Will Protect You
Therapists often prioritize their patients’ needs above their own health and safety.5,13 Their use of SPHM technology remains surprisingly low.6 One reason may be that therapists, perhaps subconsciously, believe their extensive knowledge of musculoskeletal injuries protects them during patient transfers.13
The statistics tell a different story. Surveys show that as many as 91% of practicing therapists experience work-related musculoskeletal injuries sometime during their career.1,4 Back pain leads these injuries and can be directly linked to manual lifting and transfer techniques.1,14,15 These injuries drive one in six therapists to leave the profession, while others must change work settings.16,17
When therapists work through pain, patient care suffers. Campo and colleagues conducted revealing interviews showing how injured therapists adapt their practice. One therapist admitted: “Sometimes you find yourself using or doing other things with the patients so you don’t have to transfer them.” Another confessed: “I hate to admit it, but my 4-6 pm patients might be getting gypped.”18
Working in pain leads to substandard intervention and decreased quality of care.4,15,16,18,19 Although expertise in the treatment of musculoskeletal problems is valuable, it cannot prevent therapist injuries.15,16,20 This makes mechanical aids essential, not optional, for safe patient handling.
3. Use of SPHM Techniques Is Not Consistent with Therapy Goals
Effective therapy requires active patient participation to achieve the best functional outcomes. Many therapists worry that using mechanical aids will substitute for skill development, making patients overly dependent on equipment.6 However, research shows the opposite is true.
One rehabilitation department studied this concern directly. They evaluated 47 patients at admission and discharge before implementing a SPHM program, then evaluated 47 additional patients after implementation. Patients using safe handling equipment out-performed the others in every area tested: sit-to-stand transfers, toilet transfers, tub transfers, locomotion, and stairs. Rather than hindering recovery, SPHM programs actually improved functional outcomes.21 Additional research confirmed these findings, showing that SPHM programs increase both treatment options for therapists and participation opportunities for clients.22-24
 Patients report feeling safer and more comfortable when positioned in SPHM devices. One study found that patients using safe handling devices experienced lower depression levels, improved bladder control, higher activity engagement, reduced fall risk, and increased daytime alertness.
Patients report feeling safer and more comfortable when positioned in SPHM devices. One study found that patients using safe handling devices experienced lower depression levels, improved bladder control, higher activity engagement, reduced fall risk, and increased daytime alertness.
Joyce Julien, a physical therapist at St. Elizabeth Healthcare in Kentucky, explains the shift in thinking: “Therapists need to be open-minded towards SPHM. There was some hesitancy thinking that SPHM promotes dependency because everyone is lifted and we don’t do rehab. But with implementing the use of equipment, we found that patients feel safer being moved and we can go on with rehabilitation successfully.”
Evidence-based SPHM policies are now being integrated into rehab facilities, clinics, hospitals, and schools. Therapists play a crucial role in this transformation by dispelling myths about safe patient handling. This creates safer environments that benefit both therapists and patients – the ultimate goal of quality healthcare.
References
- Pellissier B, Sarhan FR, Telliez F. Work-related, non-specific low back pain among physiotherapists in France: Prevalence and biomechanical and psychosocial risk factors, as a function of practice pattern. Int J Environ Res Public Health. 2023 28;20(5):4343. doi: 10.3390/ijerph20054343.
- Waters TR. When is it safe to manually lift a patient? Am J Nurs. 2007;107(8):53-58.
- Darragh AR, Huddleston W, King P. Work-related musculoskeletal injuries and disorders among occupational and physical therapists. Am J Occup Ther. 2009; 63(3):351-62.
- Cromie JE, Robertson VJ, Best MO. Work-related musculoskeletal disorders in physical therapists: Prevalence, severity, risks, and responses. Phys Ther. 2000; 80(4):336-51.
- Harwood K, Darragh A, Campo M, Rockefeller K, Scalzitti D. A systematic review of safe patient handling and mobility programs to prevent musculoskeletal injuries in occupational and physical therapists and assistants. IJSPHM & Falls Management 2018;8.
- Kotejoshyer R, Punnett L, Dybel G, Buchholz B. Claim costs, musculoskeletal health, and work exposure in physical therapists, occupational therapists, physical therapist assistants, and occupational therapist assistants: A comparison among long-term care jobs. Phys Ther. 2019; 99 (2):183-193. https://doi.org/10.1093/ptj/pzy137
- Marras W, Davis K, Kirking B, Bertsche P. A comprehensive analysis of low-back disorder risk and spinal loading during the transferring and repositioning of patients using different techniques. Ergonomic. 1999;42(7):904-926.
- Waters TR, Rockefeller K. Safe patient handling for rehabilitation professionals. Rehabil Nurs. 2010; 35(5):216-222.
- Darragh AR, Campo M, King P. Work-related activities associated with injury in occupational and physical therapists. Work. 2012; 42(3):373-84.
- Daynard D, Yassi A, Cooper JE, Tate R, Norman R, Wells R. Biomechanical analysis of peak and cumulative spinal loads during simulated patient–handling activities: a substudy of a randomized controlled trial to prevent lift and transfer injury of health care workers. Appl Ergon. 2001; 32(3):199-214.
- Hignett S. Intervention strategies to reduce musculoskeletal injuries associated with handling patients: a systematic review. Occup Environ Med. 2003; 69(9):e6-e6.
- Hignett S, Crumpton E, Ruszala S, Alexander P, Fray M, Fletcher B. Evidence-based patient handling: systematic review. Nurs Stand. 2003;17(33):33-6.
- Cromie JE, Robertson VJ, Best MO. Work-related musculoskeletal disorders and the culture of physical therapy. Phys Ther. 2002; 82(5):459-72
- Campo M, Weiser S, Koenig KL, Nordin M. Work-related musculoskeletal disorders in physical therapists: a Prospective cohort study with 1-year follow up. Phys Ther. 2008; 88(5); 608-19.
- Holder NL, Clark HA, DiBlasio JM, et al. Cause, prevalence, and response to occupational musculoskeletal injuries reported by physical therapists and physical therapist assistants. PhysTher. 1999; 79(7):642-52.
- West DJ, Gardner D. Occupational injuries of physiotherapists in North and Central Queensland. Aust J Physiotherapy. 2001; 47(3):179-86
- Campo M, Weiser S, Koenig KL. Job strain in physical therapists. Phys Ther. 2009; 89(9):946-56.
- Campo M, Darragh AR. Impact of work-related pain on physical therapists and occupational therapists. Phys Ther. 2010;90(6):905-920.
- Muaidi QI, Shanb AA. Prevalence causes and impact of work related musculoskeletal disorders among physical therapists. J Back Musculoskelet Rehabil. 2016.21;29(4):763-769. doi: 10.3233/BMR-160687.
- Bork BE, Cook TM, Rosecrance JC, Engelhardt KA, Thomason MJ, Wauford IJ et al. Work related musculoskeletal disorders among physical therapists. Phys Ther. 1996;6(8):827-35.
- Arnold M, Campo M, Radaweic S, Wright L. Changes in Functional Independence Measure Ratings Associated with a Safe Patient Handling and Movement Program. Rehabil Nurs. 2011;36(4):138-44.
- Campo M, Shiyko M, Margulis H, Darragh A. Effect of a Safe Patient Handling Program on Rehabilitation Outcomes. Arch Phys Med Rehabil. 2013;94(1):17-22.
- Zhuang Z, Stobbe TJ, Collins JW, Hsiao H, Hobbs G. Psychophysical assessment of assistive devices for transferring patients/residents. Appl Ergon. 2000; 31(1):35-44.
- Nelson A, Collins J, Siddharthan K, Matz M, Waters T. Link between Safe Patient Handling and Patient Outcomes in Long-Term Care. Rehabil Nurs. 2008; 33(1):33-43.