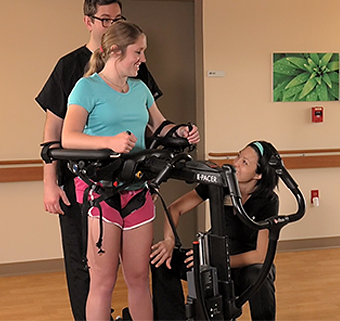Part 2: Implementing Early Mobility: The Way of the Future
ICU-Acquired Weakness and Post-Intensive Care Syndrome
| November 2020 Many patients returning home after being hospitalized for severe respiratory failure, such as those recovering from COVID-19, are now confronting significant physical, neurological, cognitive and emotional issues. To describe this wide variety of challenges, experts use the term “post-intensive care syndrome” or PICS. 1
Many patients returning home after being hospitalized for severe respiratory failure, such as those recovering from COVID-19, are now confronting significant physical, neurological, cognitive and emotional issues. To describe this wide variety of challenges, experts use the term “post-intensive care syndrome” or PICS. 1
The news media has acknowledged the increasing demand for rehabilitation during and after hospitalization. A July 2020 NBC News article states: “After any ICU stay, and particularly the lengthy ones that accompany COVID-19, most patients need to go through rehabilitation before they can regain their former strength and functioning, if they ever do. We need to be paying much more attention to how COVID-19 survivors […] are going to access the intensive rehab services they need to regain a meaningful quality of life.” 2 A June 2020 article in The Washington Post states, “The sheer size of the coronavirus pandemic means that thousands of people may need this kind of therapy…lying in an ICU, unconscious and paralyzed by powerful drugs, is harmful by itself.”3
While substantial systematic reviews of evidence-based approaches to mitigate PICS are still pending, there is growing support for the ABCDEF bundled approach to PICS prevention. Current research findings show this approach to have significant and clinically meaningful improvements in patient outcomes.4
ABCDEF
ABCDEF is an acronym for interventions that target Awakening, Breathing, Coordination of care, Delirium monitoring, Early mobilization and Family. The ABCDEF approach challenges the conventional ICU practices of deep sedation, immobilization and limited family access, and promotes channeling care resources away from passive treatments and towards early mobilization. But although early rehabilitation strategies look promising, implementing these active interventions can be difficult because of staffing limitations, financial constraints or equipment shortages.5, 6
As in so many areas involving complex patients within a heterogeneous population, early mobility and rehabilitation requires a skilled multidisciplinary team to help determine the best path for each patient. The ICU and acute care nursing and therapy staff frequently bear the primary responsibility of implementing the early mobilization and early rehabilitation protocols which often involve demanding patient transfers and mobility routines.7 This is where equipment can bridge the gap between research and practice.
Role of Equipment
Transfer and mobility devices aid the nursing and therapy staff caring for patients during ICU stays. Equipment improves the safety of the patient and decreases the physical demands on the staff during transfer and mobility tasks. When caregivers have their hands free, they can concentrate on the patient’s gait, balance and physiological response to exercise.8
Rachel Feld-Glazman, OT, MS is a Program Director at the Brain Injury Program at Burke Rehabilitation Center in White Plains, NY. Working in acute rehabilitation, her staff rehabs patients within the first two to three weeks after the onset of the medical event. “Mobilization can counteract delirium and prevent pressure sores that result from long-time in antigravity positions,” she explains. “Being physically active improves patient strength, endurance, balance and helps control blood pressure and prevent blood clots. Not only this, but we see that patient perception, cognition and orientation are improved.”
For dependent patients, walking with a traditional walker may require three or four hospital staff for safety. Fortunately, there are now several bodyweight supporting mobility devices available on the market. “Using a mobility device saves the energy of the therapist, so the therapist does not tire out and therefore can work the patient to their greater potential,” Feld-Glazman says. “With these devices, the patient has a sense of security and safety and can focus on awareness training for posture and gait.”
An untethered mobility product like the TRAM or E-Pacer allows staff to safely assist a patient in ambulation in all environments. According to Feld-Glazman, “The Rifton TRAM, for example, can go bedside and is less cumbersome when securing the patient in place. And in this mobile device, ambulation is not limited to the overhead track in the hospital gym.”
Conclusion
As we become more aware of the long-lasting impairments that are experienced by many ICU survivors, we increasingly recognize the value of early mobilization and rehabilitation for critically ill patients. The COVID-19 pandemic will add yet another dimension to this body of research.9, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26
Early mobilization and rehabilitation is an effective approach for reducing hospital length of stay, minimizing re-admissions and improving overall function of a patient, and optimizes hospital resource utilization.27 Many leading hospitals have already successfully implemented this approach. New technologies and equipment can expand opportunities for achieving the health benefits of early mobilization and rehabilitation.28
See Part 1: Understanding the Negative Impact of Prolonged ICU Care (ICU-Acquired Weakness and Post-Intensive Care Syndrome).
References
- Belluck, P. (2020, July 1). Here’s What Recovery From Covid-19 Looks Like for Many Survivors. The New York Times. https://www.nytimes.com/2020/07/01/health
- Kadakia, K. T., Nuti, S. V. and Gupta, V. (2020, July 30). Surviving a COVID-19 ICU stay is just the start. We’re ignoring what else it takes to recover. NBC News THINK. https://www.nbcnews.com/think/opinion
- Bernstein, L. (2020, June 9). Hugo Sosa survived the ICU. But for coronavirus patients like him, that’s just the start of recovery. Washington Post/Health. https://www.washingtonpost.com/health/2020
- Pun, B. T., Balas, M. C., Barnes-Daly, M. A., et al. (2019). Caring for Critically Ill Patients with the ABCDEF Bundle: Results of the ICU Liberation Collaborative in Over 15,000 Adults. Crit Care Med. 47(1):3-14. Free Full Text: https://www.ncbi.nlm.nih.gov/pmc
- Parry, S. M., Nydahl, P. and Needham, D. M. (2018). Implementing Early Physical Rehabilitation and Mobilisation in the ICU: Institutional, Clinician, and Patient Considerations. Intensive Care Med 44: 470-473. https://link.springer.com/article/10.1007%
- Dafoe, S., Chapman, M. J., Edwards, S. and Stiller, K. Overcoming Barriers to the Mobilisation of Patients in an Intensive Care Unit. Anaesth Intensive Care. Vol 43.; 2015. Free Full Text: https://journals.sagepub.com/doi/pdf/10.1177
- Krupp, A., Steege, L. and King, B. (2018). A systematic review evaluating the role of nurses and processes for delivering early mobility interventions in the intensive care unit. Intensive Crit Care Nurs. 47:30-38. Abstract https://pubmed.ncbi.nlm.nih.gov/29681432
- Hodgson, C. L., Berney, S., Harrold, M., Saxena, M. and Bellomo, R. (2013). Clinical review: Early patient mobilization in the ICU. Critical Care. 17(1): 207. Free Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles
- Dean, E., Jones, A., Peng-Ming, Yu H., Gosselink, R. and Skinner, M. (2020). Translating COVID-19 Evidence to Maximize Physical Therapists’ Impact and Public Health Response. Physical Therapy, 100(9):1458-1464. Free Full Text: https://academic.oup.com/ptj/article/100/9
- Felten-Barentsz, K. M., van Oorsouw, R., Klooster, E., Koenders, N., Driehuis, F., Hulzebos, E. H. J., van der Schaaf, M., Hoogeboom, T.J. and van der Wees, P. J. (2020). Recommendations for Hospital-Based Physical Therapists Managing Patients With COVID-19. Physical Therapy, 100(9):1444-1457. Free Full Text https://academic.oup.com/ptj/article/100/9
- Gaspari, C. H., Assumpção, I., Freire, R., Silva, A., Santiso, C. and Jaccoud, A. C. (17 September 2020). The First 60 Days: Physical Therapy in a Neurosurgical Center Converted Into a COVID-19 Center in Brazil, Physical Therapy, pzaa175, https://doi.org/10.1093/ptj/pzaa175. Free Full Text PDF: https://academic.oup.com/ptj/advance-article/doi/10.1093/ptj/pzaa175/5907857
- Iannaccone, S., Castellazzi, P., Tettamanti, A., Houdaver, E., Brugliera, L., de Blasio, F., Cimino, P., Ripa, M., Meloni, C., Alemanno, F. and Scarpellini, P. (2020). Role of Rehabilitation Department for Adult Individuals With COVID-19: The Experience of the San Raffaele Hospital of Milan. Arch Phys Med Rehabil. 2020 Sep; 101(9): 1656-1661. Published online 2020 Jun 4. doi: 10.1016/j.apmr.2020.05.015. Free Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles and https://www.archives-pmr.org/article/S0003-9993(20)30365-8/fulltext?dgcid=raven_jbs_etoc_email
- Jette, A. (n.d.) COVID-19 Virtual Issue. Physical Therapy. Oxford Academic. https://academic.oup.com/ptj/pages/covid-19
- Johnson, J. K., Lapin, B., Green, K., Stilphen, M. (28 September 2020). Frequency of Physical Therapist Intervention Is Associated With Mobility Status and Disposition at Hospital Discharge for Patients With COVID-19, Physical Therapy. Free Full Text: https://academic.oup.com/ptj/advance-article/doi/10.1093/ptj/pzaa181/5912500
- Keeney, T. (2020). Physical Therapy in the COVID-19 Pandemic: Forging a Paradigm Shift for Rehabilitation in Acute Care. Physical Therapy, 100(8):1265-1267. Free Full Text: https://academic.oup.com/ptj/article/100/8
- Korupolu, R., Francisco, G. E., Levin, H. and Needham, D. M. (2020). Rehabilitation of critically Ill COVID-19 survivors. J Int Soc Phys Rehabil. 3(2):45-52. Free Full Text (PDF) http://www.jisprm.org/article.asp?issn=2349-7904;year=2020;volume=3;issue=2
- Landry, M. D., Tupetz, A., Jalovcic, D., Sheppard, P., Jesus, T. S. and Raman, S. R. (2020, March 23). The Novel Coronavirus (COVID-19): Making a Connection between Infectious Disease Outbreaks and Rehabilitation. Physiotherapy Canada. Free Full Text https://www.utpjournals.press/doi/abs/10
- Levy, J., Léotard, A., Lawrence, C., Paquereau, J., Bensmail, D., Annane, D., Delord, V., Lofaso, F., Bessis, S. and Prigent, H. (2020). A model for a ventilator-weaning and early rehabilitation unit to deal with post-ICU impairments following severe COVID-19. Annals of Physical and Rehabilitation Medicine. 63(4):376-378. Free Full Text: https://www.sciencedirect.com/science/article
- Liu, K., Zhang, W., Yang, Y., Zhang, J., Li, Y. and Chen, L. (2020) Respiratory rehabilitation in elderly patients with COVID-19: A randomized controlled study. Complementary Therapies in Clinical Practice. 39:101166) Free Full Text: https://www.sciencedirect.com/science/article
- Rooney, S., Webster, A. and Paul, L. (2020, July 31). Systematic review of changes and recovery in physical function and fitness after severe acute respiratory syndrome-related coronavirus infection: implications for COVID-19 rehabilitation, Physical Therapy, Free Full Text: https://academic.oup.com/ptj/advance-article/doi/10.1093/ptj/pzaa129/5876270
- Sheehy, L. M. (2020). Considerations for Postacute Rehabilitation for Survivors of COVID-19. JMIR. 6(2): e19462. Free Full Text: https://pubmed.ncbi.nlm.nih.gov/32369030
- Thomas, P., Baldwin, C., Bissett, B., Boden, I., Gosselink, R., Granger, C. L., Hodgson, C., et al. (2020, April). Physiotherapy management for COVID-19 in the acute hospital setting: clinical practice recommendations. Journal of Physiotherapy. 66:2 (73-82). Free Full Text: https://www.sciencedirect.com/science/article
- Valenzuela, P. L., Joyner, M. and Lucia, A. (2020). Early mobilization in hospitalized patients with COVID-19. Ann Phys Rehabil Med. 63(4): 384-385.Free Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles
- Yang, L. and Yang, T. (2020). Pulmonary rehabilitation for patients with coronavirus disease 2019 (COVID-19), Chronic Diseases and Translational Medicine. 6(2):79-86. Free Full Text: https://www.sciencedirect.com/science/article
- Yonter, S. J., Akter, K., Bartels, M. N., Bean, J. F., Brodsky, M. B., González-Fernández, M., Henderson, D. K., Hoenig, H., Russell, H., Needham, D. M., Kumble, S. and Chan, L. (Available online 20 September 2020). What Now for Rehabilitation Specialists? Coronavirus Disease 2019 Questions and Answers. Archives of Physical Medicine and Rehabilitation. Special Communication. Full Free Text: https://www.sciencedirect.com/science/article
- Zhou, F., Yu, T., Du, R., Fan, G., Liu, Y., Liu, Z., Xiang, J., Wang, Y., Song, B., Gu, X., Guan, L., We, Y., Li, H., Wu, X., Xu, J., Tu, S., Zhang, Y., Chen, H. and Cao, B. (2020). Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 395(10229), 1054-1062. https://www.thelancet.com/journals/lancet
- Hashem, M. D., Parker, A. M. and Needham, D. M. (2016). Early Mobilization and Rehabilitation of Patients Who Are Critically Ill. Chest 150(3):722-731. Free Full Text: https://pubmed.ncbi.nlm.nih.gov/26997241
- Denehy, L., Lanphere, J. and Needham, D. M. (2017). Ten reasons why ICU patients should be mobilized early. Intensive Care Med. 43:86-90. Free Full Text: https://link.springer.com/article/10.1007/s00134-016-4513-2